Before the discovery of insulin in 1921, all people with type 1 diabetes died within a few years of being diagnosed. Although insulin is not considered a drug, its discovery was the first major breakthrough in the treatment of diabetes.
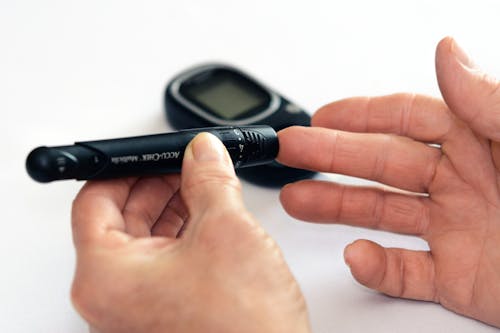
Today, healthy eating, physical activity, and insulin intake are the main treatments for type 1 diabetes. The amount of insulin must be balanced with food intake and daily activities. Your blood glucose level should be monitored carefully, checking your blood glucose level frequently. People with diabetes also have their blood glucose levels monitored several times a year with a laboratory test called A1C. The A1C test results reflect the average blood glucose level over a period of 2 to 3 months.
Healthy eating, physical activity, and blood glucose testing are essential tools in controlling type 2 diabetes. In addition, many people with type 2 diabetes need oral medications, insulin, or both to control blood glucose levels.
Get FREE access to the documentary here
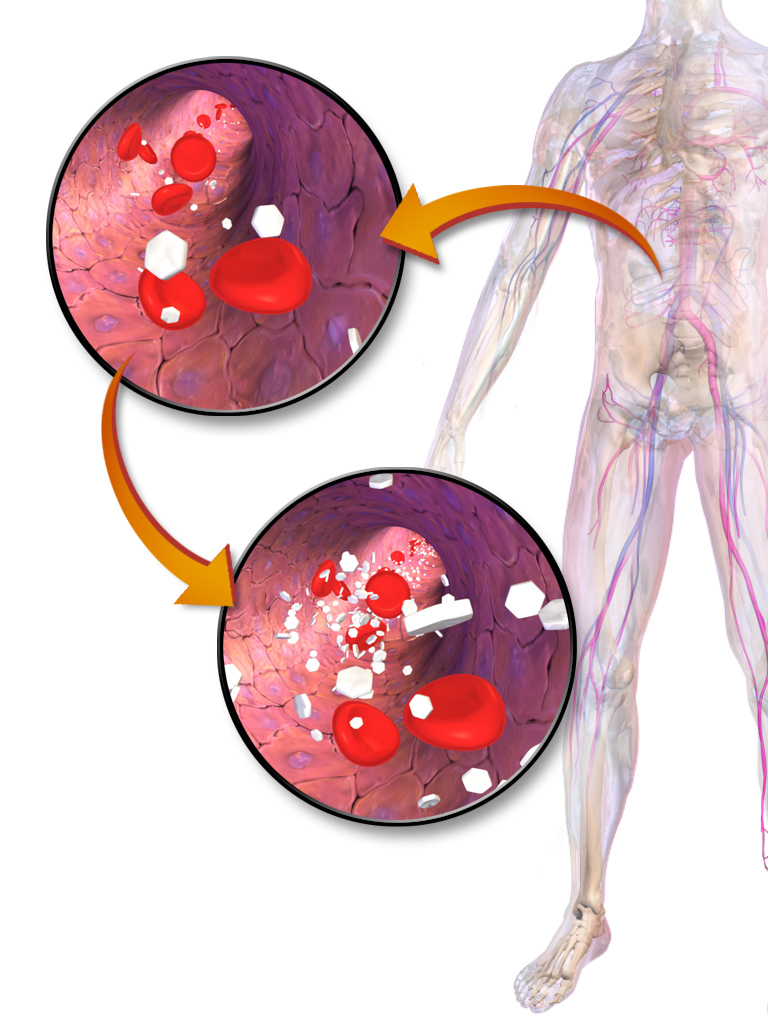
Adults with diabetes are at high risk for cardiovascular disease (CVD). In fact, at least 65% of people with diabetes die from heart disease or stroke. Controlling diabetes involves more than just controlling blood glucose levels. It is also important to control blood pressure and cholesterol levels through a healthy diet, physical activity, and medications (as needed). By doing this, people with diabetes can reduce their risk. Aspirin therapy, if recommended by healthcare professionals, and smoking cessation can also help to reduce the risk.
People with diabetes should be held responsible for their daily care. A big part of daily hygiene is preventing your blood glucose levels from getting too low or too high. When blood glucose levels drop too much - a condition known as hypoglycemia - the person can become nervous, nervous, and confused. Judgment can be impaired, and if blood glucose drops too much, fainting can occur.
A person can also get sick if blood glucose levels are too high, a condition known as hyperglycemia.
People with diabetes should consult a doctor who can help them learn how to manage and control diabetes. Most people with diabetes get help from a general practitioner, family doctor, or pediatrician. Often, having a team of doctors can improve diabetes control. The team may include:
- the attending physician, such as a general practitioner, family doctor, or pediatrician
- endocrinologist (specialist in diabetes treatment)
- nutritionist, nurse, and other health professionals who are certified diabetes trainers - specialists in providing information on diabetes care
- orthopedist (foot care)
- ophthalmologist or optometrist (for eye care)
and other health professionals, such as cardiologists and other specialists. In addition, an obstetrician specialized in caring for women with diabetes should be part of the team of pregnant women with type 1, 2, or gestational diabetes. The team may also include a pediatrician or neonatologist experienced in caring for children born to women with diabetes.
The goal of diabetes control is to keep blood glucose, blood pressure, and cholesterol levels as close as possible to the normal range. A large study, the National Institute of Diabetes, Digestive and Kidney Diseases (NIDDK) sponsored by the Diabetes and Complications Control Study (DCCT), found that keeping blood glucose levels close to normal reduces the risk of serious diabetes complications type 1. ...
This 10-year study, completed in 1993, enrolled 1,441 people with type 1 diabetes. The study compared the impact of two treatment approaches - intensive treatment and standard treatment - on the development and progression of ocular, renal, nervous, and cardiovascular complications of diabetes. . Intensive treatment aimed to keep A1C levels as close to normal as possible (6 percent). The researchers found that study participants who maintained lower blood glucose levels with intensive treatment had significantly lower rates of these complications. More recently, a follow-up study of DCCT participants showed that the ability of intensive control to reduce diabetes complications persists for more than 10 years after the trial ends.
A prospective study on diabetes in the UK, a European study completed in 1998, found that intensive control of blood glucose and blood pressure reduced the risk of blindness, kidney disease, stroke, and heart attack in people with type 2 diabetes.